Журнал «» Том 18, №3-4, 2025
Вернуться к номеру
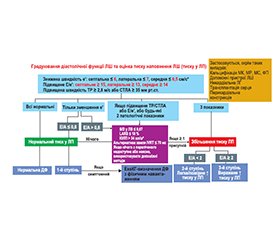
Рекомендації з ехокардіографічної оцінки діастолічної функції лівого шлуночка та діагностики серцевої недостатності зі збереженою фракцією викиду
Рубрики: Кардиология
Разделы: Справочник специалиста
Версия для печати
Рекомендації робочої групи з функціональної діагностики Асоціації кардіологів України та Всеукраїнської асоціації фахівців з ехокардіографії
Члени робочої групи з підготовки рекомендацій:
акад. НАМН України, проф. В.М. Коваленко, проф. О.С. Сичов, проф. М.М. Долженко, проф. Ю.А. Іванів, проф. О.Г. Несукай, проф. М.Ю. Колесник, д.мед.н. Л.А. Міщенко, к.мед.н. Л.Є. Лобач, к.мед.н. Т.В. Сімагіна
Список скорочень
АВ — атріовентрикулярний
АК — аортальний клапан
АР — аортальна регургітація
АС — аортальний стеноз (стеноз аортального клапана)
БНПГ — блокада ніжки пучка Гіса
ВТЛШ — вихідний тракт лівого шлуночка
ГКМП — гіпертрофічна кардіоміопатія
ГЛШ — гіпертрофія лівого шлуночка
ДКМП ...
Для ознакомления с полным содержанием статьи необходимо оформить подписку на журнал.
Список литературы
1. Nagueh SF, Smiseth OA, Appleton CP, Byrd BF 3rd, Dokainish H, Edvardsen T, et al. Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography: An Update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2016 Apr;29(4):277-314. doi: 10.1016/j.echo.2016.01.011.
2. Andersen OS, Smiseth OA, Dokainish H, Abudiab MM, Schutt RC, Kumar A, et al. Estimating left ventricular filling pressure by echocardiography. J Am Coll Cardiol. 2017;69(15):1937-48. doi: 10.1016/j.jacc.2017.01.058.
3. Inoue K, Khan FH, Remme EW, Ohte N, Garcia-Izquierdo E, Ridefelt P, et al. Determinants of left atrial reservoir and pump strain and use of atrial strain for evaluation of left ventricular filling pressure. Eur Heart J Cardiovasc Imaging. 2021;23(1):61-70. doi: 10.1093/ehjci/jeaa415.
4. Shah AM, Claggett B, Kitzman D, Biering-Srensen T, Jensen JS, Cheng S, et al. Contemporary assessment of left ventricular diastolic function in older adults: the Atherosclerosis Risk in Communities Study. Circulation. 2017;135(5):426-39. doi: 10.1161/CIRCULATIONAHA.116.024825.
5. Nagueh SF, Khan SU. Left atrial strain for assessment of left ventricular diastolic function: focus on populations with normal LVEF. JACC Cardiovasc Imaging. 2023;16(4):691-707. doi: 10.1016/j.jcmg.2022.10.011.
6. Reddy YNV, Obokata M, Egbe A, Yang JH, Pislaru S, Lin G, et al. Left atrial strain and compliance in the diagnostic evaluation of heart failure with preserved ejection fraction. Eur J Heart Fail. 2019;21(7):891-900. doi: 10.1002/ejhf.1464.
7. Kim D, Seo JH, Choi KH, Lee HY, Yang JH, Park TK, et al. Prognostic implications of left atrial stiffness index in heart failure patients with preserved ejection fraction. JACC Cardiovasc Imaging. 2023;16(3):435-45. doi: 10.1016/j.jcmg.2022.11.002.
8. Lewandowski D, Yang EY, Nguyen DT, Pandey A, Wang Z, Shah SJ, et al. Relation of left ventricular diastolic function to global fibrosis burden: implications for heart failure risk stratification. JACC Cardiovasc Imaging. 2023;16(5):783-96. doi: 10.1016/j.jcmg.2022.12.027.
9. Lababidi H, Rahi W, Smiseth OA, Billick K, Inoue K, Khan FH, et al. New algorithm for estimating left ventricular fil–ling pressure by echocardiography. Circulation. 2025 Jun 27. doi: 10.1161/CIRCULATIONAHA.125.074974.
10. Obokata M, Kane GC, Reddy YNV, Olson TP, Melenovsky V, Borlaug BA. Role of diastolic stress testing in the evaluation for heart failure with preserved ejection fraction: a simultaneous invasive-echocardiographic study. Circulation. 2017;135(9):825-38. doi: 10.1161/CIRCULATIONAHA.116.024822.
11. Ye Z, Miranda WR, Yeung DF, Lin G, Kane GC, Pislaru SV, et al. Left atrial strain in evaluation of heart failure with preserved ejection fraction. J Am Soc Echocardiogr. 2020;33(12):1490-9. doi: 10.1016/j.echo.2020.07.020.
12. Merli E, Ciampi Q, Scali MC, Simova I, Podlesnikar T, Bossone E, et al. Pulmonary congestion during exercise stress echocardiography in ischemic and heart failure patients. Circ Cardiovasc Imaging. 2022;15(3):e013558. doi: 10.1161/CIRCIMAGING.121.013558.
13. Choi EY, Shim CY, Kim SA, Cho IJ, Ha JW, Kim YJ, et al. Passive leg-raise is helpful to identify impaired diastolic functional reserve during exercise in patients with abnormal myocardial relaxation. J Am Soc Echocardiogr. 2010;23(5):523-30. doi: 10.1016/j.echo.2010.02.004.
14. Luong CL, Anand V, Padang R, Miranda WR, Kane GC, Obokata M, et al. Prognostic significance of elevated left ventricular filling pressures with exercise: insights from a cohort of 14,338 patients. J Am Soc Echocardiogr. 2024;37(4):382-93.e1. doi: 10.1016/j.echo.2023.11.012.
15. Jiang R, Yeung DF, Behnami D, Miranda WR, Pislaru SV, Kane GC, et al. A novel continuous left ventricular diastolic function score using machine learning. J Am Soc Echocardiogr. 2022;35(9):1247-55. doi: 10.1016/j.echo.2022.06.005.
16. Lee E, Ito S, Miranda WR, Lin G, Reddy YNV, Obokata M, et al. Artificial intelligence-enabled ECG for left ventricular diastolic function and filling pressure. NPJ Digit Med. 2024;7:4.
17. Chao CJ, Kato N, Scott CG, Pellikka PA, Kane GC, Miranda WR, et al. Unsupervised machine learning for assessment of left ventricular diastolic function and risk stratification. J Am Soc Echocardiogr. 2022;35(10):1214-25.e8. doi: 10.1016/j.echo.2022.06.013.
18. Avenatti E, Little SH, Barker CM, et al. Changes in left atrial function after transcutaneous mitral valve repair. Am J Cardiol. 2018;122(7):1204-9. doi: 10.1016/j.amjcard.2018.06.031.
19. Zaid RR, Barker CM, Little SH, et al. Pre- and post-operative diastolic dysfunction in patients with valvular heart disease: diagnosis and therapeutic implications. J Am Coll Cardiol. 2013;62(21):1922-30. doi: 10.1016/j.jacc.2013.08.1619.
20. Ito S, Miranda WR, Nkomo VT, Boler AN, Pislaru SV, Pellikka PA, et al. Prognostic risk stratification of patients with moderate aortic stenosis. J Am Soc Echocardiogr. 2021;34(3):248-56. doi: 10.1016/j.echo.2020.10.012.
21. Smiseth OA, Morris DA, Cardim N, Cikes M, Fraser AG, Flachskampf FA, et al. Multimodality imaging in patients with heart failure and preserved ejection fraction: an expert consensus document of the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging. 2022;23(5):e34-e61. doi: 10.1093/ehjci/jeab154.
22. Liu D, Hu K, Niemann Phelan D, Collier P, Thavendiranathan P, et al. Relative apical sparing of longitudinal strain using two-dimensional speckle-tracking echocardiography is both sensitive and specific for the diagnosis of cardiac amyloidosis. Heart. 2012;98(19):1442-8.
23. Liu D, Hu K, Niemann M, et al. Effect of combined systolic and diastolic functional parameter assessment for differentiation of cardiac amyloidosis from other causes of concentric left ventricular hypertrophy. Circ Cardiovasc Imaging. 2013;6(6):1066-72. doi: 10.1161/CIRCIMAGING.113.000683.
24. Pagourelias ED, Mirea O, Duchenne J, et al. Echo para–meters for differential diagnosis in cardiac amyloidosis: A head-to-head comparison of deformation and nondeformation parameters. Circ Cardiovasc Imaging. 2017;10(10):e005588. doi: 10.1161/CIRCIMAGING.116.005588.
25. Kusunose K, Dahiya A, Popovic ZB, et al. Biventricular mechanics in constrictive pericarditis comparison with restrictive cardiomyopathy and impact of pericardiectomy. Circ Cardiovasc Imaging. 2013;6:399-406. doi: 10.1161/CIRCIMAGING.112.000078.
26. Klein AL, Wang TKM, Cremer PC, et al. Pericardial di–seases: International position statement on new concepts and advances in multimodality cardiac imaging. JACC Cardiovasc Ima–ging. 2024;17(5):937-88. doi: 10.1016/j.jcmg.2024.04.010.
27. Qamruddin S, Alkharabsheh SK, Sato K, et al. Differentiating constriction from restriction (from the Mayo clinic echocardiographic criteria). Am J Cardiol. 2019;124:932-8. doi: 10.1016/j.amjcard.2019.06.002.
28. Wada Y, Murata K, Tanaka T, et al. Simultaneous Doppler tracing of transmitral inflow and mitral annular velocity as an estimate of elevated left ventricular filling pressure in patients with atrial fibrillation. Circ J. 2012;76:675-81. doi: 10.1253/circj.cj-11-0703.
29. Goyal P, Almarzooq ZI, Horn EM, et al. Characteristics of hospitalizations for heart failure with preserved ejection fraction. Am J Med. 2016;129:635.e15-26. doi: 10.1016/j.amjmed.2016.02.007.
30. Sharma K, Kass DA. Heart failure with preserved ejection fraction: Mechanisms, clinical features, and therapies. Circ Res. 2014;115:79-96. doi: 10.1161/CIRCRESAHA.115.302922.
31. Yancy CW, Jessup M, Bozkurt B, et al. 2017 ACC/AHA/HFSA focused update of the 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Task force on clinical practice guidelines and the Heart Failure Society of America. Circulation. 2017;136:e137-e61. doi: 10.1161/CIR.0000000000000509.
32. Lfstrm U, Hage C, Savarese G, et al. Prognostic impact of Framingham heart failure criteria in heart failure with preserved ejection fraction. ESC Heart Failure. 2019;6:830-9. doi: 10.1002/ehf2.12458.
33. Reddy YNV, Carter RE, Obokata M, et al. A simple, evidence-based approach to help guide diagnosis of heart failure with preserved ejection fraction. Circulation. 2018;138:861-70. doi: 10.1161/CIRCULATIONAHA.118.034646.
34. Rahi W, Hussain I, Nguyen DT, et al. Accuracy of clinical evaluation and chest X-ray for HFpEF diagnosis: comparison against right heart catheterization. Am J Cardiol. 2023;206:219-20. doi: 10.1016/j.amjcard.2023.08.112.
35. Pieske B, Tschpe C, de Boer RA, Fraser AG, Anker SD, Donal E, et al. How to diagnose heart failure with preserved ejection fraction: the HFA-PEFF diagnostic algorithm: a consensus recommendation from the Heart Failure Association (HFA) of the European Society of Cardiology (ESC). Eur J Heart Fail. 2020 Mar;22(3):391-412. doi: 10.1002/ejhf.1741.
36. Chow SL, Maisel AS, Anand I, et al. Role of Biomarkers for the Prevention, assessment, and management of heart failure: a scientific statement from the American Heart Association. Circulation. 2017;135:e1054-91. doi: 10.1161/CIR.0000000000000490.
37. Anjan VY, Loftus TM, Burke MA, et al. Prevalence, clinical phenotype, and outcomes associated with normal B-type natriuretic peptide levels in heart failure with preserved ejection fraction. Am J Cardiol. 2012;110:870-6. doi: 10.1016/j.amjcard.2012.05.014.
38. Gonzlez-Lpez E, Gallego-Delgado M, Guzzo-Merel-lo G, et al. Wildtype transthyretin amyloidosis as a cause of heart failure with preserved ejection fraction. Eur Heart J. 2015;36:2585-94. doi: 10.1093/eurheartj/ehv338.
39. Hahn VS, Yanek LR, Vaishnav J, et al. Endomyocardial biopsy characterization of heart failure with preserved ejection fraction and prevalence of cardiac amyloidosis. JACC Heart Fail. 2020;8:712-24. doi: 10.1016/j.jchf.2020.04.007.